Abstract
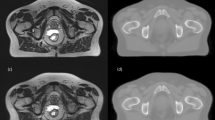
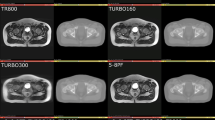
Objective To enhance the opacity function for computed tomography (CT)-based prostate volume rendered (VR) images using reference magnetic resonance (MR) images.
Materials and Methods After simulating on phantoms, ten patients with CT and MR datasets were identified/ registered. Optimal VR images were produced, and intra-modality and cross-modality errors [mean distance in voxel units (VU) from VR partial surface to target] were computed. On the CT VR images, a global transformation was computed to relate the opacity functions obtained using CT reference volumes with those obtained using MR reference volumes.
Results The prostate was better visualized on MR than CT, as the intra-modality errors obtained using MR (2.78 ± 1.02 VU) were lower than on CT (3.68 ± 2.15 VU). Despite similar qualitative results as the intra-modality CT images, the cross-modality errors obtained using the individual patient data (2.77 ± 0.99 VU) and using the global transformation (2.89 ± 0.99 VU) were each closer (P = 0.010 and P = 0.011, respectively) to the intra-modality MR errors than were the intra-modality CT errors.
Conclusion By optimizing the opacity function using MR reference images, CT VR images of the prostate could closely represent the prostate defined on MR; furthermore, this process can be approximated by a simple transformation. Overall, the errors were reduced to a level (<3 VU) justifying further exploration in CT-based radiotherapy treatment planning.
Similar content being viewed by others
References
Jani AB, Hellman S (2003) Early prostate cancer: clinical decision-making. Lancet 361:1045–1053
Horwitz EM, Hanks GE (2000) External beam radiation therapy for prostate cancer. CA Cancer J Clin 50:349–375
Hanks GE, Lee WR, Hanlon AL et al (1996) Conformal technique dose escalation for prostate cancer: biochemical evidence of improved cancer control with higher doses in patients with pretreatment prostate-specific antigen >10 ng/ml. Int J Radiat Oncol Biol Phys 35:862–868
Barth N (1990) An inverse treatment planning problem in radiation therapy. Int J Radiat Oncol Biol Phys 18:425–41
Jani AB, Roeske JC, Rash C (2003) Intensity-modulated radiation therapy for prostate cancer. Clin Prostate Cancer 2:98–105
Hanley J, Lumley MA, Mageras GS et al (1997) Measurement of patient positioning errors in three-dimensional conformal radiotherapy of the prostate. Int J Radiat Oncol Biol Phys 37:435–444
Beard CJ, Kijewski P, Bussiere M et al (1996) Analysis of prostate and seminal vesicle motion: implications for treatment planning. Int J Radiat Oncol Biol Phys 34:451–458
Cazzaniga LF, Marinoni MA, Bossi A et al (1998) Interphysician variability in defining the planning target volume in the irradiation of the prostate and seminal vesicles. Radiother Oncol 47:293–296
Fiorino C, Reni M, Bolognesi A et al (1998) Intra- and inter-observer variability in contouring prostate and seminal vesicles: implications for conformal treatment planning. Radiother Oncol 47:285–292
Valicenti RK, Sweet JW, Hauck WW et al (1999) Variation of clinical target volume definition in three-dimensional conformal radiation therapy for prostate cancer. Int J Radiat Oncol Biol Phys 44:931–935
Lebesque JV, Bruce AM, Kroes AP et al (1995) Variation in volumes, dose-Volume histograms, and estimated normal tissue complication probabilities of rectum and bladder during conformal radiotherapy of T3 prostate cancer. Int J Radiat Oncol Biol Phys 33:1109–1119
Chen LM, Lubich L, Chiru P et al (1996) Localization of the prostatic apex for radiotherapy planning: a comparison of two techniques. Br J Radiol 69:821–829
Sweeney PJ, Vijayakumar S, Sibley GS et al (1993) Comparison of CT-based treatment planning and retrograde urethography in determining the prostatic apex at simulation. Med Dosim 18:21–28
Jani AB, Sychra JJ (1994) MR image classification algorithms for neurosurgical and stereotactic radiosurgical trajectory planning and volumetric analysis. Neurol Res 16:17–23
Ramsey CR, Oliver AL (1998) Magnetic resonance imaging based digitally reconstructed radiographs, virtual simulation, and three-dimensional treatment planning. Med Phys 25:1928–1934
Ramsey CR, Arwood D, Scaperoth D et al (1999) Clinical application of digitally-reconstructed radiographs generated from magnetic resonance imaging for intracranial lesions. Int J Radiat Oncol Biol Phys 45:797–802
Yin FF, Gao Q, Xie H et al (1998) MR image-guided portal verification for brain treatment field. Int J Radiat Oncol Biol Phys 40:703–711
Lee YK, Bollet M, Charles-Edwards G et al (2003) Radiotherapy treatment planning of prostate cancer using magnetic resonance imaging alone. Radiother Oncol 66:203–216
Mah D, Steckner M, Hanlon A et al (2002) MRI simulation: effect of gradient distortions on three-dimensional prostate cancer plans. Int J Radiat Oncol Biol Phys 53:757–765
Steenbakkers RJ, Deurloo KE, Nowak PJ et al (2003) Reduction of dose delivered to the rectum and bulb of the penis using MRI delineation for radiotherapy of the prostate. Int J Radiat Oncol Biol Phys 57:1269–1279
Khoo VS, Dearnaley DP, Finnigan DJ et al (1997) Magnetic resonance imaging (MRI): considerations and applications in radiotherapy treatment planning. Radiother Oncol 42:1–15
Drebin RA, Carpenter L, Hanrahan P (1988) Volume rendering. Comput Graph 22(4):65–74
Rubin GD, Napel S, Leung AN (1996) Volumetric analysis of volumetric data: achieving a paradigm shift. Radiology 200:312–317
Ney DR, Fishman EK, Magid D et al (1990) Volumetric rendering of computed tomography data: principles and practice. IEEE Comput Graph Appl 9:24–32
Scatarige JC, Urban BA, Hellmann DB et al (2001) Three-dimensional volume-rendering CT angiography in vasculitis: spectrum of disease and clinical utility. J Comput Assist Tomogr 25:598–603
Rubin GD, Beaulieu CF, Argiro V et al (1996) Perspective volume rendering of CT and MR images: applications for endoscopic imaging. Radiology 200:564–568
Salgado R, Mulkens T, Bellinck P et al (2003) Volume rendering in clinical practice. a pictorial review. JBR-BTR 86:215–220
Udupa JK, Hung HM, Chuang KS (1991) Surface and volume rendering in 3D imaging: a comparison. J Digital Imag 4:159–168
Hohme KH, Hanson WA (1992) Interactive 3D-segmentation of MRI and CT volume using morphological operations. J Comput Assist Tomogr 16:285–294
Pallotta S, Bucciolini M, Russo S et al (2006) Accuracy evaluation of image registration and segmentation tools used in conformal treatment planning of prostate cancer. Comput Med Imaging Graph 30:1–7
Kniss J, Kindlmann G, Hansen C (2002) Multi-dimensional transfer functions for interactive volume rendering. IEEE Trans Vis Comput Graph 8:270–285
Sato Y, Westing A, Bhalerao S et al (2000) Tissue classification based on 3D local intensity structures for volume rendering. IEEE Trans Vis Comput Graph 6:160–179
Laidlaw DH, Fleischer KW, Barr AH (1998) Partial-volume Bayesian classification of material mixture in MR volume data using voxel histograms. IEEE Trans Med Imag 17:74–86
Souza A, Udupa JK, Saha PK (2005) Volume rendering in the presence of partial volume effects. IEEE Trans Med Imaging 24:223–235
Foley JD, Van Dam A, Feiner SK et al (1990) Viewing in three dimensions. In: Computer graphics: principles and practice, 2nd edn. Addison-Wesley, Reading, pp 229–283
Jani AB, Pelizzari CA, Chen GTY et al (1997) Interactive tool for evaluating the utility of volume-rendered images versus sagittal plane-picked images of the prostate for radiotherapy treatment planning. RSNA Electronic J 1:http://ej. rsna.org
Jani AB, Pelizzari CA, Chen GTY et al (1998) Accuracy of object depiction and opacity transfer function optimization in CT volume-rendered images. J Comput Assist Tomogr 22:459–470
Jani AB, Pelizzari CA, Chen GTY et al (2000) Volume rendering quantification algorithm for reconstruction of CT volume rendered structures: I. Cerebral arteriovenous malformations. IEEE Trans Med Imaging 19:12–24
Jani AB, Irick JS, Pelizzari C (2005) Opacity transfer function optimization for volume-rendered computed tomography images of the prostate. Acad Radiol 12:761–770
Paliwal BR, Ritter MA, McNutt TR et al (1998) A solid water pelvic and prostate phantom for imaging, volume rendering, treatment planning, and dosimetry for an RTOG multi-institutional, 3-D dose escalation study. Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys 42: 205–211
Powell MJD (1964) An efficient method for finding the minimum of a function of several variables without calculating derivatives. Comput J 7:155–163
Kindlmann G, Durkin JW (1998) Semi-automatic generation of transfer functions for direct volume rendering. In: Proceedings of IEEE Symposium on Volume Visualization, pp 79–86
Chen L, Price RA Jr, Wang L et al (2004) MRI-based treatment planning for radiotherapy: dosimetric verification for prostate IMRT. Int J Radiat Oncol Biol Phys 60:636–647
Chen GT, Pelizzari CA, Levin DN (1990) Image correlation in oncology. Important Adv Oncol 1:131–141
Dawson-Saunders B, Trapp RG (1990) Basic and clinical biostatistics. Prentice Hall, East Norwalk
Lee EK, Fox T, Crocker I (2006) Simultaneous beam geometry and intensity map optimization in intensity-modulated radiation therapy. Int J Radiat Oncol Biol Phys 64:301–320
Author information
Authors and Affiliations
Corresponding author
Additional information
Grant Support: This work was supported by an American Society of Therapeutic Radiology and Oncology (ASTRO) Junior Faculty Research Grant/Award, and was an oral presentation at the annual meeting of ASTRO in Philadelphia, PA in November 2006.
Rights and permissions
About this article
Cite this article
Jani, A.B., Johnstone, P.A.S., Fox, T. et al. Optimization of opacity function for computed tomography volume rendered images of the prostate using magnetic resonance reference volumes. Int J CARS 1, 285–293 (2007). https://doi.org/10.1007/s11548-006-0065-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-006-0065-1