Abstract
Purpose
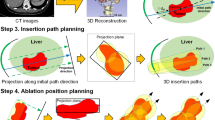
Preoperative treatment planning is key to ensure successful thermal ablation of liver tumors. The planning aims to minimize the number of electrodes required for complete ablation and the damage to the surrounding tissues while satisfying multiple clinical constraints. This is a challenging multiple objective planning problem, in which the trade-off between different objectives must be considered.
Methods
We propose a novel method to solve the multiple objective planning problem, which combines the set cover-based model and Pareto optimization. The set cover-based model considers multiple clinical constraints and generates several clinically feasible treatment plans, among which the Pareto optimization is performed to find the trade-off between different objectives.
Results
We evaluated the proposed method on 20 tumors of 11 patients in two different situations used in common thermal ablation approaches: with and without the pull-back technique. Pareto optimal plans were found and verified to be clinically acceptable in all cases, which can find the trade-off between the number of electrodes and the damage to the surrounding tissues.
Conclusion
The proposed method performs well in the two different situations we considered: with or without the pull-back technique. It can generate Pareto optimal plans satisfying multiple clinical constraints. These plans consider the trade-off between different planning objectives.






Similar content being viewed by others
References
Daher S, Massarwa M, Benson AA, Khoury T (2018) Current and future treatment of hepatocellular carcinoma: an updated comprehensive review. J Clin Transl Hepatol 6(1):69
Hinshaw JL, Lubner MG, Ziemlewicz TJ, Lee FT Jr, Brace CL (2014) Percutaneous tumor ablation tools: microwave, radiofrequency, or cryoablation—what should you use and why? Radiographics 34(5):1344–1362
Rhim H, Lim HK, Ys K, Choi D, Lee WJ (2008) Radiofrequency ablation of hepatic tumors: lessons learned from 3000 procedures. J Gastroenterol Hepatol 23(10):1492–1500
Lyons GR, Pua BB (2019) Ablation planning software for optimizing treatment: challenges, techniques, and applications. Tech Vasc Interv Radiol 22(1):21–25
Schumann C, Rieder C, Bieberstein J, Weihusen A, Zidowitz S, Moltz JH, Preusser T (2010) State of the art in computer-assisted planning, intervention, and assessment of liver-tumor ablation. Crit Revi™ Biomed Eng 38(1):31–52
Villard C, Soler L, Papier N, Agnus V, Gangi A, Mutter D, Marescaux J (2003) RF-Sim: a treatment planning tool for radiofrequency ablation of hepatic tumors. Paper presented at the Proceedings on Seventh International Conference on Information Visualization, 2003. IV 2003.,
Altrogge I, Kröger T, Preusser T, Büskens C, Pereira PL, Schmidt D, Weihusen A, Peitgen H-O (2006) Towards optimization of probe placement for radio-frequency ablation. Paper presented at the International Conference on Medical Image Computing and Computer-Assisted Intervention,
Schumann C, Bieberstein J, Trumm C, Schmidt D, Bruners P, Niethammer M, Hoffmann RT, Mahnken AH, Pereira PL, Peitgen H-O (2010) Fast automatic path proposal computation for hepatic needle placement. Paper presented at the Medical Imaging 2010: Visualization, Image-Guided Procedures, and Modeling,
Seitel A, Engel M, Sommer CM, Radeleff BA, Essert-Villard C, Baegert C, Fangerau M, Fritzsche KH, Yung K, Meinzer HP (2011) Computer-assisted trajectory planning for percutaneous needle insertions. Med Phys 38(6):3246–3259
Schumann C, Rieder C, Haase S, Teichert K, Süss P, Isfort P, Bruners P, Preusser T (2015) Interactive multi-criteria planning for radiofrequency ablation. Int J Comput Assist Radiol Surg 10(6):879–889
Peters T, Clark J, Pike G, Henri C, Collins L, Leksell D, Jeppsson O (1989) Stereotactic neurosurgery planning on a personal-computer-based work station. J Digit Imaging 2(2):75
Essert C, Haegelen C, Lalys F, Abadie A, Jannin P (2012) Automatic computation of electrode trajectories for deep brain stimulation: a hybrid symbolic and numerical approach. Int J Comput Assist Radiol Surg 7(4):517–532
De Momi E, Caborni C, Cardinale F, Casaceli G, Castana L, Cossu M, Mai R, Gozzo F, Francione S, Tassi L, Lo Russo G, Antiga L, Ferrigno G (2014) Multi-trajectories automatic planner for StereoElectroEncephaloGraphy (SEEG). Int J Comput Assist Radiol Surg 9(6):1087–1097
Sparks R, Vakharia V, Rodionov R, Vos SB, Diehl B, Wehner T, Miserocchi A, McEvoy AW, Duncan JS, Ourselin S (2017) Anatomy-driven multiple trajectory planning (ADMTP) of intracranial electrodes for epilepsy surgery. Int J Comput Assist Radiol Surg 12(8):1245–1255
Chen M-H, Yang W, Yan K, Zou M-W, Solbiati L, Liu J-B, Dai Y (2004) Large liver tumors: protocol for radiofrequency ablation and its clinical application in 110 patients—mathematic model, overlapping mode, and electrode placement process. Radiology 232(1):260–271
Yang L, Wen R, Qin J, Chui C-K, Lim K-B, Chang SK-Y (2010) A robotic system for overlapping radiofrequency ablation in large tumor treatment. IEEE ASME Trans Mechatron 15(6):887
Ren H, Campos-Nanez E, Yaniv Z, Banovac F, Abeledo H, Hata N, Cleary K (2014) Treatment planning and image guidance for radiofrequency ablation of large tumors. IEEE J Biomed Health Inform 18(3):920–928
Ren H, Guo W, Ge SS, Lim W (2014) Coverage planning in computer-assisted ablation based on genetic algorithm. Comput Biol Med 49:36–45
Jaberzadeh A, Essert C (2016) Pre-operative planning of multiple probes in three dimensions for liver cryosurgery: comparison of different optimization methods. Math Methods Appl Sci 39(16):4764–4772
Chen R, Lu F, Wang K, Kong D (2018) Semi-automatic radiofrequency ablation planning based on constrained clustering process for hepatic tumors. IEEE Trans Biomed Eng 65(3):645–657
Liang L, Cool D, Kakani N, Wang G, Ding H, Fenster A (2019) Automatic radiofrequency ablation planning for liver tumors with multiple constraints based on set covering. IEEE Trans Med Imaging 39(5):1459–1471
Keanini R, Rubinsky B (1992) Optimization of multiprobe cryosurgery. J Heat Transf 114(4):796–801
Baissalov R, Sandison GA, Reynolds D, Muldrew K (2001) Simultaneous optimization of cryoprobe placement and thermal protocol for cryosurgery. Phys Med Biol 46(7):1799
Giorgi G, Avalle L, Brignone M, Piana M, Caviglia G (2013) An optimisation approach to multiprobe cryosurgery planning. Comput Methods Biomech Biomed Eng 16(8):885–895
Torricelli M, Ferraguti F, Secchi C (2013) An algorithm for planning the number and the pose of the iceballs in cryoablation. Paper presented at the 2013 35th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC),
Granna J, Nabavi A, Burgner-Kahrs J (2019) Computer-assisted planning for a concentric tube robotic system in neurosurgery. Int J Comput Assist Radiol Surg 14(2):335–344
Cepek J, Lindner U, Davidson SR, Haider MA, Ghai S, Trachtenberg J, Fenster A (2014) Treatment planning for prostate focal laser ablation in the face of needle placement uncertainty. Med Phys 41:013301
Liang L, Cool D, Kakani N, Wang G, Ding H, Fenster A (2019) Development of a multi-objective optimized planning method for microwave liver tumor ablation. Paper presented at the International Conference on Medical Image Computing and Computer-Assisted Intervention,
GAMS - The Solver Manuals, GAMS Release 25.1.3 (2018). GAMS Development Corporation Washington, DC, USA. https://www.gams.com/25.1/docs/S_CPLEX.html
Emmerich MT, Deutz AH (2018) A tutorial on multiobjective optimization: fundamentals and evolutionary methods. Nat Comput 17(3):585–609
Bilic P, Christ PF, Vorontsov E, Chlebus G, Chen H, Dou Q, Fu C-W, Han X, Heng P-A, Hesser JJapa (2019) The liver tumor segmentation benchmark (lits). arXiv:1901.04056
Chan C, Tan S (2001) Determination of the minimum bounding box of an arbitrary solid: an iterative approach. Comput Struct 79(15):1433–1449
Audigier C, Mansi T, Delingette H, Rapaka S, Mihalef V, Sharma P, Carnegie D, Boctor E, Choti M, Kamen A (2013) Lattice Boltzmann method for fast patient-specific simulation of liver tumor ablation from CT images. Paper presented at the International Conference on Medical Image Computing and Computer-Assisted Intervention,
Mariappan P, Weir P, Flanagan R, Voglreiter P, Alhonnoro T, Pollari M, Moche M, Busse H, Futterer J, Portugaller HR (2017) GPU-based RFA simulation for minimally invasive cancer treatment of liver tumours. Int J Comput Assist Radiol Surg 12(1):59–68
Huang Q, Ding H, Wang X, Wang G (2018) Robust extraction for low-contrast liver tumors using modified adaptive likelihood estimation. Int J Comput Assist Radiol Surg 13(10):1565–1578
Huang Q, Ding H, Wang X, Wang G (2018) Fully automatic liver segmentation in CT images using modified graph cuts and feature detection. Comput Biol Med 95:198–208
Huang Q, Sun J, Ding H, Wang X, Wang G (2018) Robust liver vessel extraction using 3D U-Net with variant dice loss function. Comput Biol Med 101:153–162
Funding
This work was supported by National Key R&D Program of China (2019YFC0119503, 2017YFA0205904) and Tsinghua University Initiative Scientific Research Program (20197010009).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
This article used public dataset.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This paper is based on the work: “Liang L., Cool D., Kakani N., Wang G., Ding H., Fenster A. (2019) Development of a Multi-objective Optimized Planning Method for Microwave Liver Tumor Ablation. In: Shen D. et al. (eds) Medical Image Computing and Computer Assisted Intervention – MICCAI 2019. MICCAI 2019. Lecture Notes in Computer Science, vol 11768. Springer, Cham.”
Rights and permissions
About this article
Cite this article
Liang, L., Cool, D., Kakani, N. et al. Multiple objective planning for thermal ablation of liver tumors. Int J CARS 15, 1775–1786 (2020). https://doi.org/10.1007/s11548-020-02252-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-020-02252-6