Abstract
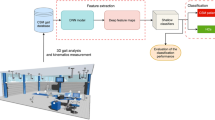
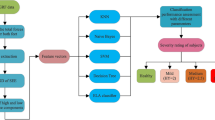
Cervical spondylotic myelopathy (CSM) is the main cause of cervical spinal cord dysfunction in adults, especially in middle-aged and elderly patients, which easily leads to gait disturbance. In the present study, we propose a dynamic method for the detection of CSM based on nonlinear dynamics of gait system and deterministic learning theory. First, a 3-dimensional (3D) gait analysis system is used to capture the walking locomotion from healthy controls (HCs) and patients with CSM. Discriminant kinematic gait features, including angles of hip and knee joints in the sagittal and coronal planes, are extracted based on statistical analysis and clinicians’ empirical investigation. Second, deterministic learning theory is used to model and identify nonlinear gait system dynamics of HCs and patients with CSM, which are approximated and stored in constant Radial Basis Function (RBF) neural networks (NN). The disparity of gait system dynamics between the two groups of participants is used for classification and detection of the presence of CSM by constructing a bank of dynamic estimators with constant RBF NN. Finally, experiments are carried out on the self-constructed CSM gait database to evaluate the performance of the proposed method, in which gait data from 45 CSM patients and 45 age-matched HCs are involved. By using 2-fold and leave-one-out cross-validation styles, the achieved average classification accuracy is reported to be 94.44\(\%\) and 95.56\(\%\), respectively. The results demonstrate excellent performance and the proposed method has the potential to serve as a candidate for the automatic detection of CSM in clinical examination.



Similar content being viewed by others
Data availability
The datasets generated during the current study are available from the corresponding author on reasonable request.
References
Bohm PE, Fehlings MG, Kopjar B, Tetreault LA, Vaccaro AR, Anderson KK, Arnold PM (2017) Psychometric properties of the 30-m walking test in patients with degenerative cervical myelopathy: results from two prospective multicenter cohort studies. Spine J 17(2):211–217
Chakraborty J, Nandy A (2020) Discrete wavelet transform based data representation in deep neural network for gait abnormality detection. Biomed Signal Process Control 62:102076
de Oliveira Assis A, Rodrigues FB, Carafini A, Lemes TS, de Villa GAG, de Oliveira Andrade A, Vieira MF (2020) Influence of sampling frequency and number of strides on recurrence quantifiers extracted from gait data. Comput Biol Med 119:103673
Erickson BJ (2017) Machine learning: discovering the future of medical imaging. J Digital Imaging 30:391
Haddas R, Ju KL (2019) Gait alteration in cervical spondylotic myelopathy elucidated by ground reaction forces. Spine 44(1):25–31
Haddas R, Ju KL, Patel S, Belanger TA, Arakal RG (2017) Altered ground reaction forces in adult cervical spondylotic myelopathy compared to controls. Spine J 17(10):S44
Haddas R, Lieberman I, Arakal R, Boah A, Belanger T, Ju K (2018) Effect of cervical decompression surgery on gait in adult cervical spondylotic myelopathy patients. Clin Spine Surg 31(10):435–440
Haddas R, Patel S, Arakal R, Boah A, Belanger T, Ju KL (2018) Spine and lower extremity kinematics during gait in patients with cervical spondylotic myelopathy. Spine J 18(9):1645–1652
Haddas R, Cox J, Belanger T, Ju KL, Derman PB (2019) Characterizing gait abnormalities in patients with cervical spondylotic myelopathy: a neuromuscular analysis. Spine J 19(11):1803–1808
Hayfron-Acquah JB, Nixon MS, Carter JN (2003) Automatic gait recognition by symmetry analysis. Pattern Recogn Lett 24(13):2175–2183
Hopkins BS, Weber KA II, Kesavabhotla K, Paliwal M, Cantrell DR, Smith ZA (2019) Machine learning for the prediction of cervical spondylotic myelopathy: a post hoc pilot study of 28 participants. World Neurosurg 127:e436–e442
Huo H, Chang Y, Tang Y (2022) Analysis of treatment effect of acupuncture on cervical spondylosis and neck pain with the data mining technology under deep learning. J Supercomput 78(4):5547–5564
Hussain VS, Spano ML, Lockhart TE (2020) Effect of data length on time delay and embedding dimension for calculating the Lyapunov exponent in walking. J R Soc Interface 17(168):20200311
Kalsi-Ryan S, Rienmueller AC, Riehm L, Chan C, Jin D, Martin AR, Fehlings MG (2020) Quantitative assessment of gait characteristics in degenerative cervical myelopathy: a prospective clinical study. J Clin Med 9(3):752
Karadimas SK, Erwin WM, Ely CG, Dettori JR, Fehlings MG (2013) Pathophysiology and natural history of cervical spondylotic myelopathy. Spine 38(22S):S21–S36
Karadimas SK, Moon ES, Yu WR, Satkunendrarajah K, Kallitsis JK, Gatzounis G, Fehlings MG (2013) A novel experimental model of cervical spondylotic myelopathy (CSM) to facilitate translational research. Neurobiol Dis 54:43–58
Khan O, Badhiwala JH, Grasso G, Fehlings MG (2020) Use of machine learning and artificial intelligence to drive personalized medicine approaches for spine care. World Neurosurg 140:512–518
Khan O, Badhiwala JH, Witiw CD, Wilson JR, Fehlings MG (2021) Machine learning algorithms for prediction of health-related quality-of-life after surgery for mild degenerative cervical myelopathy. Spine J 21(10):1659–1669
Kitade I, Nakajima H, Takahashi A, Matsumura M, Shimada S, Kokubo Y, Matsumine A (2020) Kinematic, kinetic, and musculoskeletal modeling analysis of gait in patients with cervical myelopathy using a severity classification. Spine J 20(7):1096–1105
Koyama T, Fujita K, Watanabe M, Kato K, Sasaki T, Yoshii T, Okawa A (2022) Cervical myelopathy screening with machine learning algorithm focusing on finger motion using noncontact sensor. Spine 47(2):163–171
Malone A, Meldrum D, Bolger C (2015) Three-dimensional gait analysis outcomes at 1 year following decompressive surgery for cervical spondylotic myelopathy. Eur Spine J 24(1):48–56
McCormick JR, Sama AJ, Schiller NC, Butler AJ, Donnally CJ (2020) Cervical spondylotic myelopathy: a guide to diagnosis and management. J Am Board Fam Med 33(2):303–313
McDermott A, Bolger C, Keating L, McEvoy L, Meldrum D (2010) Reliability of three-dimensional gait analysis in cervical spondylotic myelopathy. Gait Posture 32(4):552–558
Merali ZG, Witiw CD, Badhiwala JH, Wilson JR, Fehlings MG (2019) Using a machine learning approach to predict outcome after surgery for degenerative cervical myelopathy. PLoS ONE 14(4):e0215133
Merali Z, Wang JZ, Badhiwala JH, Witiw CD, Wilson JR, Fehlings MG (2021) A deep learning model for detection of cervical spinal cord compression in MRI scans. Sci Rep 11(1):1–11
Phinyomark A, Larracy R, Scheme E (2020) Fractal analysis of human gait variability via stride interval time series. Front Physiol 11:333
Sreeraj M, Joy J, Jose M, Varghese M, Rejoice TJ (2022) Comparative analysis of Machine Learning approaches for early stage Cervical Spondylosis detection. J King-Saudi Univ 34(6):3301–3309
Tapia C, Daud O, Ruiz-del-Solar J (2017) EMG signal filtering based on independent component analysis and empirical mode decomposition for estimation of motor activation patterns. J Med Biol Eng 37(1):140–155
ur Rehman N, Aftab H (2019) Multivariate variational mode decomposition. IEEE Trans Signal Process 67(23):6039–6052
Wang C, Hill DJ (2006) Learning from neural control. IEEE Trans Neural Netw 17(1):130–146
Wang C, Hill DJ (2007) Deterministic learning and rapid dynamical pattern recognition. IEEE Trans Neural Netw 18(3):617–630
Wang C, Hill DJ (2009) Deterministic Learning Theory for Identification, Recognition and Control. CRC Press, Boca Raton, FL
Wang S, Hu Y, Shen Y, Li H (2018) Classification of diffusion tensor metrics for the diagnosis of a myelopathic cord using machine learning. Int J Neural Syst 28(02):1750036
Wang N, Luo C, Huang X, Huang Y, Zhan J (2021) DeepCS: Training a deep learning model for cervical spondylosis recognition on small-labeled sensor data. Neurocomputing 472:24–34
Yentes JM, Raffalt PC (2021) Entropy analysis in gait research: methodological considerations and recommendations. Ann Biomed Eng 49:979–990
Yonenobu K, Abumi K, Nagata K, Taketomi E, Ueyama K (2001) Interobserver and Intraobserver reliability of the Japanese Orthopaedic association scoring system for evaluation of cervical compression myelopathy. Spine 26(17):1890–1894
Yu X, Xiang L (2014) Classifying cervical spondylosis based on fuzzy calculation. Abs Appl Anal 2014:2014
Yu X, Liu M, Meng L, Xiang L (2015) Classifying cervical spondylosis based on x-ray quantitative diagnosis. Neurocomputing 165:222–227
Acknowledgements
Not applicable.
Funding
This work was supported by the National Natural Science Foundation of China (Grant No. 62,173,212) and by the Natural Science Foundation of Fujian Province (Grant No. 2022J011146).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
There is no conflict of interest.
Ethical approval
The present study was approved by the ethical review board (KYLL-2020(KS)-743).
Consent to participate
Informed consent was obtained from all participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ji, B., Dai, Q., Ji, X. et al. Detection of cervical spondylotic myelopathy based on gait analysis and deterministic learning. Artif Intell Rev 56, 9157–9173 (2023). https://doi.org/10.1007/s10462-023-10404-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10462-023-10404-8