Abstract
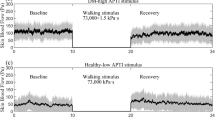
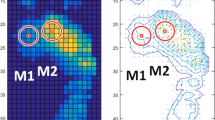
The aim of this study was to investigate the plantar blood flow response to the same accumulated pressure stimulus in diabetic patients with different peak plantar pressure (PPP), which is important for assessing the risk of diabetic foot ulcer. Eleven diabetic subjects with high PPP (PPP ≥ 207 kPa) and 8 diabetic subjects with low PPP (PPP < 207 kPa) were asked to walk naturally on a treadmill so as to induce an accumulated stimulus of 73,000 kPa·s on their first metatarsal head, which was monitored with a sensorized insole. Blood perfusion (BP) in the first metatarsal head was measured before and after walking. Results showed that blood flow after applying the same walking stimulus was significantly decreased in comparison to the basal BP before walking in both high PPP and low PPP groups (p < 0.05), but no significant differences were found between the two groups in terms of BP parameters and its percentage change (p > 0.05). Moreover, BP parameters were not significantly correlated to PPP and the pressure-time integral (PTI) of the subjects’ gait (p > 0.05). This indicated that, besides PPP and PTI, the accumulated mechanical stimulus should be taken into consideration when assessing the risk of diabetic patients developing foot ulcers.

Plantar blood flow response to a walking stimulus




Similar content being viewed by others
References
Actis RL, Ventura LB, Lott DJ, Smith KE, Commean PK, Hastings MK, Mueller MJ (2008) Multi-plug insole design to reduce peak plantar pressure on the diabetic foot during walking. Med Biol Eng Comput 46:363–371. https://doi.org/10.1007/s11517-008-0311-5
Arts ML, Waaijman R, De HM, Keukenkamp R, Nollet F, Bus SA (2012) Offloading effect of therapeutic footwear in patients with diabetic neuropathy at high risk for plantar foot ulceration. Diabetic Med 29:1534–1541. https://doi.org/10.1111/j.1464-5491.2012.03770.x
Carter MR, Mcginn R, Barreraramirez J, Sigal RJ, Kenny GP (2014) Impairments in local heat loss in type 1 diabetes during exercise in the heat. Med Sci Sports Exerc 46:2224–2233
Caselli A, Pham H, Giurini JM, Armstrong DG, Veves A (2002) The forefoot-to-rearfoot plantar pressure ratio is increased in severe diabetic neuropathy and can predict foot ulceration. Diabetes Care 25:1066–1071. https://doi.org/10.2337/diacare.24.10.1810
Chao CY, Cheing GL (2009) Microvascular dysfunction in diabetic foot disease and ulceration. Diabetes Metab Res Rev 25:604–614. https://doi.org/10.1002/dmrr.1004
Charanya G, Patil KM, Narayanamurthy VB, Parivalavan R, Visvanathan K (2004) Effect of foot sole hardness, thickness and footwear on foot pressure distribution parameters in diabetic neuropathy. Proc Inst Mech Eng H 218:431–443. https://doi.org/10.1243/0954411042632117
Colberg SR, Parson HK, Nunnold T, Holton DR, Swain DP, Vinik AI (2005) Change in cutaneous perfusion following 10 weeks of aerobic training in Type 2 diabetes. J Diabetes Complicat 19:276–283. https://doi.org/10.1016/j.jdiacomp.2005.02.006
Colberg SR, Sigal RJ, Fernhall B, Regensteiner JG, Blissmer BJ, Rubin RR, Chasan-Taber L, Albright AL, Braun B (2010) Exercise and type 2 diabetes: the American College of Sports Medicine and the American Diabetes Association: joint position statement executive summary. Diabetes Care 33:e147–e167. https://doi.org/10.2337/dc10.1548
Dixit S, Maiya AG, Shastry BA (2014) Effect of aerobic exercise on peripheral nerve functions of population with diabetic peripheral neuropathy in type 2 diabetes: a single blind, parallel group randomized controlled trial. J Diabetes Complicat 28:332–339. https://doi.org/10.1016/j.jdiacomp.2013.12.006
Fromy B, Abraham P, Bouvet C, Bouhanick B, Fressinaud P, Saumet JL (2002) Early decrease of skin blood flow in response to locally applied pressure in diabetic subjects. Diabetes 51:1214–1217. https://doi.org/10.2337/diabetes.51.4.1214
Gärtner V, Eigentler TK (2008) Pathogenesis of diabetic macro- and microangiopathy. Clin Nephrol 70:1–9
Guldemond NA, Leffers P, Walenkamp GH, Schaper NC, Sanders AP, Nieman FH, van Rhijn LW (2008) Prediction of peak pressure from clinical and radiological measurements in patients with diabetes. BMC Endocr Disord 8:16
Hsi WL, Chai HM, Lai JS (2002) Comparison of pressure and time parameters in evaluating diabetic footwear. Am J Phys Med Rehab 81:822–829. https://doi.org/10.1097/01.PHM.0000030724.45454.5C
Jan Y-K, Shen S, Foreman RD, Ennis WJ (2013) Skin blood flow response to locally applied mechanical and thermal stresses in the diabetic foot. Microvasc Res 89:40–46. https://doi.org/10.1016/j.mvr.2013.05.004
Jan YK, Lung CW, Cuaderes E, Rong D, Boyce K (2013) Effect of viscoelastic properties of plantar soft tissues on plantar pressures at the first metatarsal head in diabetics with peripheral neuropathy. Physiol Meas 34:53–66. https://doi.org/10.1088/0967-3334/34/1/53
Lalli P, Chan A, Garven A, Midha N, Chan C, Brady S, Block E, Hu B, Toth C (2013) Increased gait variability in diabetes mellitus patients with neuropathic pain. J Diabetes Complicat 27:248–254. https://doi.org/10.1016/j.jdiacomp.2012.10.013
Lavery LA, Armstrong DG, Wunderlich RP, Tredwell J, Boulton AJ (2003) Predictive value of foot pressure assessment as part of a population-based diabetes disease management program. Diabetes Care 26:1069–1073. https://doi.org/10.2337/diacare.26.4.1069
Mayrovitz HN, Macdonald J, Smith JR (1999) Blood perfusion hyperaemia in response to graded loading of human heels assessed by laser-Doppler imaging. Clin Physiol 19:351–359
Mueller MJ, Tuttle LJ, Lemaster JW, Strube MJ, Mcgill JB, Hastings MK, Sinacore DR (2013) Weight-bearing versus nonweight-bearing exercise for persons with diabetes and peripheral neuropathy: a randomized controlled trial. Arch Phys Med Rehabil 94:829–838. https://doi.org/10.1016/j.apmr.2012.12.015
Newton DJ, Bennett SP, Fraser J, Khan F, Belch JJ, Griffiths G, Leese GP (2005) Pilot study of the effects of local pressure on microvascular function in the diabetic foot. Diabetic Med 22:1487–1491. https://doi.org/10.1111/j.1464-5491.2005.01659.x
Owings T, Apelqvist J, Stenström A, Becker M, Bus S, Kalpen A, Ulbrecht J, Cavanagh P (2009) Plantar pressures in diabetic patients with foot ulcers which have remained healed. Diabetic Med 26:1141–1146. https://doi.org/10.1111/j.1464-5491.2009.02835.x
Paton JS, Stenhouse EA, Bruce G, Zahra D, Jones RB (2012) A comparison of customised and prefabricated insoles to reduce risk factors for neuropathic diabetic foot ulceration: a participant-blinded randomised controlled trial. J Foot Ankle Res 5:1–11. https://doi.org/10.1186/1757-1146-5-31
Patry J, Belley R, Côté M, Chateau-Degat M-L (2013) Plantar pressures, plantar forces, and their influence on the pathogenesis of diabetic foot ulcers: a review. J Am Podiatr Med Assoc 103:322–332
Periyasamy R, Anand S, Ammini A (2012) Investigation of Shore meter in assessing foot sole hardness in patients with diabetes mellitus—a pilot study. Int J Diabetes Dev C 32:169–175
Petrofsky JS, Bains GS, Prowse M, Mc LK, Ethiraju G, Lee S, Gunda S, Lohman E, Schwab E (2009) The influence of age and diabetes on the skin blood flow response to local pressure. Med Sci Monit 15:CR325–CR331
Pu F, Fan X, Yang Y, Chen W, Li S, Li D, Fan Y (2014) Feedback system based on plantar pressure for monitoring toe-walking strides in children with cerebral palsy. Am J Phys Med Rehab 93:122–129. https://doi.org/10.1097/PHM.0b013e3182a54207
Sartor CD, Hasue RH, Cacciari LP, Butugan MK, Watari R, Pássaro AC, Giacomozzi C, Sacco IC (2014) Effects of strengthening, stretching and functional training on foot function in patients with diabetic neuropathy: results of a randomized controlled trial. Bmc Musculoskel Dis 15:1–13. https://doi.org/10.1186/1471-2474-15-137
Stoa EM, Meling S, Nyhus L-K, Stromstad G, Mangerud KM, Helgerud J, Bratland-Sanda S, Storen O (2017) High-intensity aerobic interval training improves aerobic fitness and HbA1c among persons diagnosed with type 2 diabetes. Eur J Appl Physiol 117:455–467. https://doi.org/10.1007/s00421-017-3540-1
Tuttle LJ, Hastings MK, Mueller MJ (2012) A moderate-intensity weight-bearing exercise program for a person with type 2 diabetes and peripheral neuropathy. Phys Ther 92:133–141. https://doi.org/10.2522/ptj.20110048
Waaijman R, Bus SA (2012) The interdependency of peak pressure and pressure-time integral in pressure studies on diabetic footwear: no need to report both parameters. GaitPosture 35(1):1–5. https://doi.org/10.1016/j.gaitpost.2011.07.006
Funding
This work was supported by the National Natural Science Foundation of China [grant number 11672027] and Beijing Municipal Science & Technology Commission [grant number Z171100000517010].
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of Beihang University and with the Declaration of Helsinki. Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Pu, F., Ren, W., Fu, H. et al. Plantar blood flow response to accumulated pressure stimulus in diabetic people with different peak plantar pressure: a non-randomized clinical trial. Med Biol Eng Comput 56, 1127–1134 (2018). https://doi.org/10.1007/s11517-018-1836-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-018-1836-x