Abstract
Purpose
Free fibula flap is the gold standard for the treatment of mandibular defects. However, the existing preoperative planning protocol is cumbersome to execute, costly to learn, and poorly collaborative with the robot-assisted cutting of the fibular osteotomy plane.
Methods
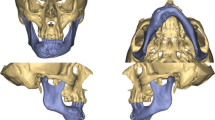
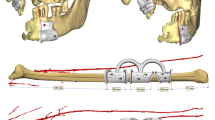
A surgical planning system for robotic assisted mandibular reconstruction with fibula free flap is proposed in this study. A fibular osteotomy planning algorithm is presented so that the virtual surgical planning of the fibular osteotomy segments can be obtained automatically with selected mandibular anatomical landmarks. The planned osteotomy planes are then converted into the motion path of the robotic arm, and the automatic fibula osteotomy is completed under optical navigation.
Results
Surgical planning was performed on 35 patients to verify the feasibility of our system’s virtual surgical planning module, with an average time of 13 min. Phantom experiments were performed to evaluate the reliability and stability of this system. The average distance and angular deviations of the osteotomy planes are 1.04 ± 0.68 mm and 1.56 ±1.10°, respectively.
Conclusions
Our system can achieve not only precise and convenient preoperative planning, but also safe and reliable osteotomy trajectory. The clinical applications of our system for mandibular reconstruction surgery are expected soon.










Similar content being viewed by others
References
Papadopulos NA, Schaff J, Sader R, Kovacs L, Deppe H, Kolk A, Biemer E (2008) Mandibular reconstruction with free osteofasciocutaneous fibula flap: a 10 years experience. Injury Int J Care Inj 39(3):75–82. https://doi.org/10.1016/j.injury.2008.05.017
Irjala H, Kinnunen I, Aitasalo K (2012) Mandibular reconstruction using free bone flap after preoperative chemoradiation. Eur Arch Otorhinolaryngol 269:1513–1518. https://doi.org/10.1007/s00405-011-1795-4
Patel A, Harrison P, Cheng A, Bray B, Bell RB (2019) Fibular reconstruction of the maxilla and mandible with immediate implant-supported prosthetic rehabilitation: jaw in a day—sciencedirect. Oral Maxillofac Surg Clin N Am 31(3):369–386. https://doi.org/10.1016/j.coms.2019.03.002
Lee SW, Kim HG, Ham MJ, Hong DK, Kim SG, Rotaru H (2017) Custom implant for reconstruction of mandibular continuity defect. J Oral Maxillofac Surg Off J Am Assoc Oral Maxillofac Surg. https://doi.org/10.1016/j.joms.2017.12.003
Kim JW, Hwang JH, Ahn KM (2016) Fibular flap for mandible reconstruction in osteoradionecrosis of the jaw: selection criteria of fibula flap. Maxillofac Plast Reconstr Surg 38(1):46. https://doi.org/10.1186/s40902-016-0093-x
Ni Y, Ping L, Yang Z, Wang W, Dai W, Qi Z, Duan W, Xu Z, Sun C, Liu F (2018) The application of fibular free flap with flexor hallucis longus in maxilla or mandible extensive defect: a comparison study with conventional flap. World J Surg Oncol 16(1):149. https://doi.org/10.1186/s12957-018-1450-2
Yu Y, Zhang WB, Liu XJ, Guo CB, Yu GY, Peng X (2016) Three-dimensional accuracy of virtual planning and surgical navigation for mandibular reconstruction with free fibula flap. J Oral Maxillofac Surg 1503:e1-1503.e10. https://doi.org/10.1016/j.joms.2016.02.020
Craig ES, Yuhasz M, Shah A, Blumberg J, Steinbacher DM (2015) Simulated surgery and cutting guides enhance spatial positioning in free fibular mandibular reconstruction. Microsurgery 35(1):29–33. https://doi.org/10.1002/micr.22229
Qu X, Zhen W, Hui SO, Zhang C, Abdelrehem A (2020) Accuracy of computer-aided design/computer-aided manufacturing surgical template for guidance of dental implant distraction in mandibular reconstruction with free fibula flaps. J Craniofac Surg 31(2):355–359. https://doi.org/10.1097/SCS.0000000000006112
Maesschalck TD, Courvoisier DS, Scolozzi P (2017) Computer-assisted versus traditional freehand technique in fibular free flap mandibular reconstruction: a morphological comparative study. Eur Arch Oto-Rhino-Laryngol 274:517–526. https://doi.org/10.1007/s00405-016-4246-4
Brandt SA, Walter U, Reimers CD, Schreiber SJ, Thömke F, Urban PP (2014) Computer-assisted mandibular reconstruction using a patient-specific reconstruction plate fabricated with computer-aided design and manufacturing techniques. Craniomaxillofac Trauma Reconstr 07(02):158–166. https://doi.org/10.1055/s-0034-1371356
Mascha F, Winter K, Pietzka S, Heufelder M, Schramm A, Wilde F (2017) Accuracy of computer-assisted mandibular reconstructions using patient-specific implants in combination with CAD/CAM fabricated transfer keys. J Cranio-Maxillofac Surg 45(11):1884–1897. https://doi.org/10.1016/j.jcms.2017.08.028
Sieira Gil R, Marí Roig A, Arranz Obispo C, Morla A, Martí Pagès C, Llopis Perez J (2015) Surgical planning and microvascular reconstruction of the mandible with a fibular flap using computer-aided design, rapid prototype modelling, and precontoured titanium reconstruction plates: a prospective study. Br J Oral Maxillofac Surg 53(1):49–53. https://doi.org/10.1016/j.bjoms.2014.09.015
Farfalli GL, Albergo JI, Ritacco LE, Ayerza MA, Milano FE, Aponte-Tinao LA (2017) What is the expected learning curve in computer-assisted navigation for bone tumor resection. Clin Orthop Relat Res 475(3):668–675. https://doi.org/10.1007/s11999-016-4761-z
Ni Y, Zhang X, Meng Z, Li Z, Li S, Xu Z, Sun C, Liu F, Duan W (2021) Digital navigation and 3D model technology in mandibular reconstruction with fibular free flap: a comparative study. J Stomatol Oral Maxillofac Surg 122(4):e59–e64. https://doi.org/10.1016/j.jormas.2020.11.002
Hanasono MM, Skoracki RJ (2013) Computer-assisted design and rapid prototype modeling in microvascular mandible reconstruction. Laryngoscope 123:597–604. https://doi.org/10.1002/lary.23717
Kong X, Duan X, Wang Y (2016) An integrated system for planning, navigation and robotic assistance for mandible reconstruction surgery. Intell Serv Robot 9:113–121. https://doi.org/10.1007/s11370-015-0189-7
Cheng L, Carriere J, Piwowarczyk J, Aalto D, Zemiti N, de Boutray M, Tavakoli M (2021) Admittance-controlled robotic assistant for fibula osteotomies in mandible reconstruction surgery. Adv Intell Syst 3:2000158. https://doi.org/10.1002/aisy.202000158
Chao AH, Weimer K, Raczkowsky J, Zhang Y, Kunze M, Cody D, Selber JC, Hanasono MM, Skoracki RJ (2016) Pre-programmed robotic osteotomies for fibula free flap mandible reconstruction: a preclinical investigation. Microsurgery 36:246–249. https://doi.org/10.1002/micr.30013
Goetze E, Gielisch M, Moergel M, Al-Nawas B (2017) Accelerated workflow for primary jaw reconstruction with microvascular fibula graft. 3D Print Med 3(1):3. https://doi.org/10.1186/s41205-017-0010-7
Goormans F, Sun Y, Bila M, Schoenaers J, Geusens J, Lübbers H-T, Coucke W, Politis C (2019) Accuracy of computer-assisted mandibular reconstructions with free fibula flap: results of a single-center series. Oral Oncol 97:69–75. https://doi.org/10.1016/j.oraloncology.2019.07.022
Zhao H, Tian J (2015) Study on a medical robot for Mandible Reconstruction Surgery. In: 2015 IEEE international conference on mechatronics and automation (ICMA), pp 1513–1518. https://doi.org/10.1109/ICMA.2015.7237709
Pietruski P, Majak M, Światek-Najwer E, Żuk M, Popek M, Mazurek M, Świecka M, Jaworowski J (2019) Navigation-guided fibula free flap for mandibular reconstruction: a proof of concept study. J Plast Reconstr Aesthet Surg 72(4):572–580. https://doi.org/10.1016/j.bjps.2019.01.026
Xu J, Liu J, Zhang D, Zhou Z, Zhang C, Chen X (2021) A 3D segmentation network of mandible from CT scan with combination of multiple convolutional modules and edge supervision in mandibular reconstruction. Comput Biol Med 138:104925. https://doi.org/10.1016/j.compbiomed.2021.104925
Lorensen WE, Cline HE (1987) Marching cubes: a high resolution 3d surface construction algorithm. ACM Siggraph Comput Graph 21(4):163–169. https://doi.org/10.1145/37402.37422
Li Y, Hu J, Tao B et al (2020) Automatic robot-world calibration in an optical-navigated surgical robot system and its application for oral implant placement. Int J Comput Assist Radiol Surg. https://doi.org/10.1007/s11548-020-02232-w
Besl PJ, McKay ND (1992) Method for registration of 3-D shapes. In: Sensor fusion IV: control paradigms and data structures, vol 1611. [S.l.: s.n.], pp 586–606 https://doi.org/10.1109/34.121791
Jewer DD, Boyd JB, Manktelow RT et al (1989) Orofacial and mandibular reconstruction with the iliac crest free flap: a review of 60 cases and a new method of classification. Plast Reconstr Surg 84:391–403. https://doi.org/10.1097/00006534-198909000-00002
West JB, Fitzpatrick JM, Toms SA, Maurer CR Jr, Maciunas RJ (2001) Fiducial point placement and the accuracy of point-based, rigid body registration. Neurosurgery 48(4):810–816. https://doi.org/10.1097/00006123-200104000-00023
Tehrani JN, O’brien RT, Poulsen PR et al (2013) Real-time estimation of prostate tumor rotation and translation with a kV imaging system based on an iterative closest point algorithm. Phys Med Biol 58(23):8517–8533. https://doi.org/10.1118/1.4815469
Seginer A (2011) Rigid-body point-based registration: the distribution of the target registration error when the fiducial registration errors are given. Med Image Anal 15(4):397–413. https://doi.org/10.1016/j.media.2011.01.001
Chen Y, Pang L, Hu L, Yu T, Wang W (2013) Rapid prototyping technique applied to surgical guidance of second reconstruction surgery of defective mandible. In: 2013 IEEE 3rd Portuguese meeting in bioengineering (ENBENG). IEEE, pp 1–5. https://doi.org/10.1109/ENBENG.2013.6518418
Li P, Xuan M, Liao C, Tang W, Wang X-Y, Tian W, Long J (2016) Application of intraoperative navigation for the reconstruction of mandibular defects with microvascular fibular flaps-preliminary clinical experiences. J Craniofac Surg 27(3):751–755. https://doi.org/10.1097/SCS.0000000000002430
Yu Y, Zhang WB, Liu XJ, Guo CB, Yu GY, Peng X (2020) Selection of guiding plate combined with surgical navigation for microsurgical mandibular reconstruction. J Craniofac Surg 31(4):960–965. https://doi.org/10.1097/SCS.0000000000006295
Plessers K, Verhaegen F, Van Dijck C, Wirix-Speetjens R, Debeer P, Jonkers I, Sloten JV (2020) Automated quantification of glenoid bone defects using 3-dimensional measurements. J Should Elbow Surg 29(5):1050–1058. https://doi.org/10.1016/j.jse.2019.10.007
Vanden Berghe P, Demol J, Gelaude F, Vander Sloten J (2017) Virtual anatomical reconstruction of large acetabular bone defects using a statistical shape model. Comput Methods Biomech Biomed Eng 20:577–586. https://doi.org/10.1080/10255842.2016.1265110
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (81971709; M-0019; 82011530141), the Foundation of Science and Technology Commission of Shanghai Municipality (20490740700), Shanghai Jiao Tong University Foundation on Medical and Technological Joint Science Research (YG2019ZDA06; YG2021ZD21; YG2021QN72; YG2022QN056), and Hospital Funded Clinical Research (21XJMR02), Xinhua Hospital Affiliated to Shanghai Jiao Tong University, School of Medicine.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
There was no informed consent required for the work reported in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guo, Y., Xu, W., Tu, P. et al. Design and implementation of a surgical planning system for robotic assisted mandible reconstruction with fibula free flap. Int J CARS 17, 2291–2303 (2022). https://doi.org/10.1007/s11548-022-02748-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-022-02748-3